 THE HPO AXIS (Hypothalamic-Pituitary-Ovarian axis):
THE HPO AXIS (Hypothalamic-Pituitary-Ovarian axis):
Hormonal control of the menstrual cycle/ Feedback Mechanism:
The events of the menstrual cycle are controlled by an interplay of five hormones secreted by three organs and known as the hypothalamic-pituitary- ovarian-axis, (HPO axis). (Fig. 6-6).
The three organs are:
(i) the Hypothalamus at the base of the brain which secretes gonadotropic releasing hormone (GnRH),
(ii) the Pituitary gland, a tiny gland just below the hypothalamus which secretes follicle stimulating hormone (FSH) and luteinizing hormone (LH),
(iii) the Ovaries which secretes the steroid hormones oestrogen and progesterone.
The interplay of hormones in the HPO axis is regulated by a feedback mechanism.
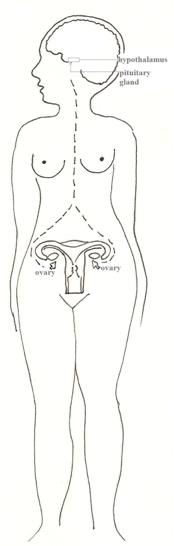
<< Fig. 6-6; The HPO Axis: The three organs of the H-P-O axis are the hypothalamus at the base of the brain, the pituitary gland just below it and the ovaries, one on each side of the pelvis. (Diagram courtesy of Mary Kane)
Feedback Mechanism – role of the hypothalamus and pituitary gland, (Fig. 6-7):
The gonadotropin hormones FSH and LH are secreted by the pituitary gland. FSH is necessary for the development of the immature ovum, (i.e. the primordial follicle in the ovary), and LH triggers ovulation. The secretion of FSH and LH from the pituitary gland is under the control of gonadotropin releasing hormone (GnRH) from the hypothalamus, and the hypothalamus in turn is controlled by the levels of the ovarian steroid hormones oestrogen and progesterone in the blood by means a feedback mechanism. The hypothalamus may also be affected by external factors e.g. stress. (see topic ‘Factors that interfere with the interpretation of mucus’ under the ‘Cervical Mucus’ heading).
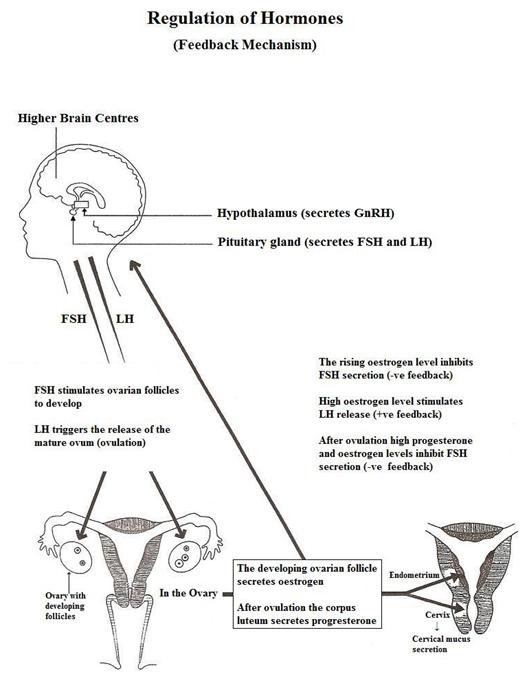
Fig 6-7; The hypothalamic-pituitary-ovarian axis (HPO axis) and feedback mechanism: As oestrogen and progesterone levels are low at the beginning of the cycle this allows follicle stimulating hormone (FSH) to be released from the pituitary gland under the stimulation of Gonadotropin Releasing Hormone (GnRH) from the hypothalamus. FSH stimulates a number of ovarian follicles to develop. The growing follicles in the ovary secrete oestrogen which causes proliferation of the endometrium (proliferative phase of the endometrium),and secretion of cervical mucus. The rising oestrogen from the developing follicles suppresses FSH secretion in order to inhibit development of any new follicles, (negative feedback mechanism). By day 7 of an average 28 day cycle one of the developing follicles becomes dominant (Graafian follicle), and the others regress. The high oestrogen from the dominant follicle stimulates the secretion of luteinizing hormone (LH surge) from the pituitary (positive feedback) which triggers ovulation. After ovulation the ruptured follicle become the corpus luteum which secretes progesterone and oestrogen. Progesterone stimulates further development of the endometrium to prepare for possible pregnancy, (secretory phase of the endometrium), and stimulates the glands in the cervical crypts to secrete gestogenic G mucus which occludes the cervical canal. The high progesterone and oestrogen levels in the luteal phase suppress FSH secretion (negative feedback). If pregnancy does not occur the corpus luteum regresses 14 days after ovulation and the drop in progesterone causes sloughing of the endometrium (menstruation). The low oestrogen and progesterone at the beginning of the cycle allows the suppression of FSH to be lifted and a new cycle begins. (Diagram courtesy of Fergal Mulcahy) (See Diagram on Changes in different organs during the menstrual cycle, Page 9 in http://Pictures & Diagrams )
THE FEEDBACK MECHANISM – WHAT IS HAPPENING IN THE OVARY (Fig. 6-7)


